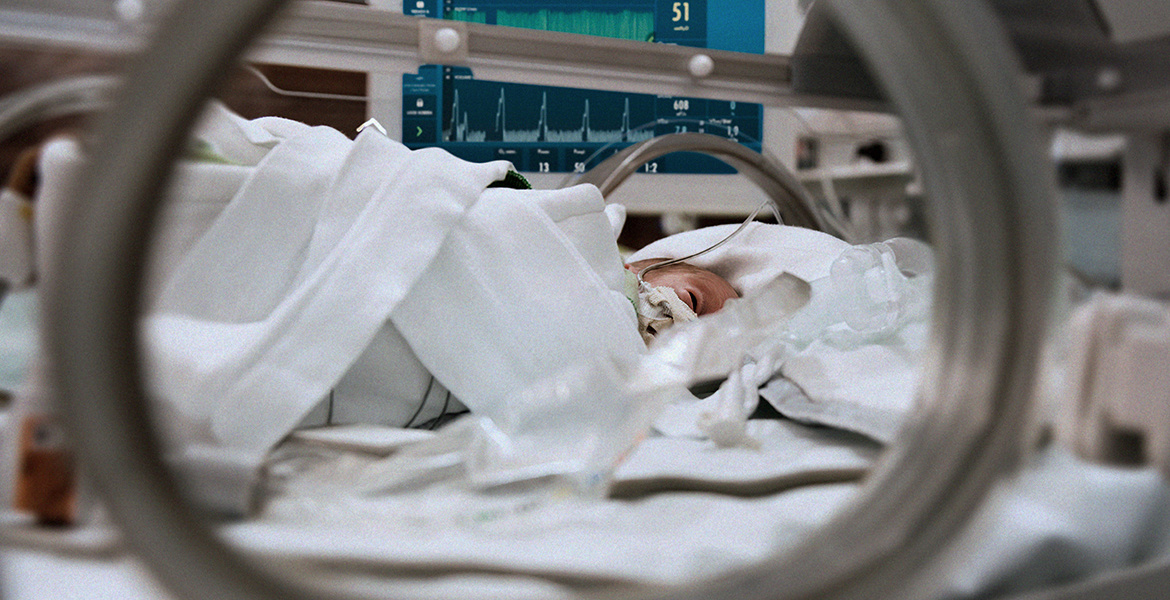
Born 12 weeks too early with 50/50 chance at survival, Sabina Checketts has grown up to become a neonatal doctor herself, using new therapies and sophisticated technology to improve outcomes for premature babies. One such technique, invented by Getinge, applies sensors to help babies on ventilators breathe more easily and naturally—and it's increasingly being used on adults. It's just one part of a quiet revolution in intensive care.
When Sabina Checketts holds her hand a certain way, the tiny scar on the back of it looks like a rocket ship. Checketts got the scar during the first few days of her life, during a tenuous struggle for survival, after she was born at 28 weeks—12 weeks prematurely. Her rocket ship scar, and a few other small ones, are marks left by lines inserted into her tiny, frail body to keep her alive.
I don't point these out to parents, but to me they're badges of honor, because I survived.

The parents she's referring to are parents of her patients. Thirty-three years after her early birth, Checketts now works as a neonatal doctor. Today, she uses vastly improved technologies and techniques to create better outcomes for other premature babies—and more hope for their parents.
As vulnerable premature babies fight to stay alive one of the most critical issues is something most people never think twice about—breathing. A pivotal advance in neonatal medicine—and one that has a major impact in adult critical care—has been the development of better ventilators.
"One of the main challenges for premature babies is with ventilation," says Checketts. "Their lungs are quite stiff when they're first born because they're so immature. They're very fragile."
The ventilator that helped Checketts survive was a far cry from what she sees today when she treats premature babies. "We've gone from a mode of ventilation where you were breathing for the baby to one now where we can breathe with the baby as well," she says.
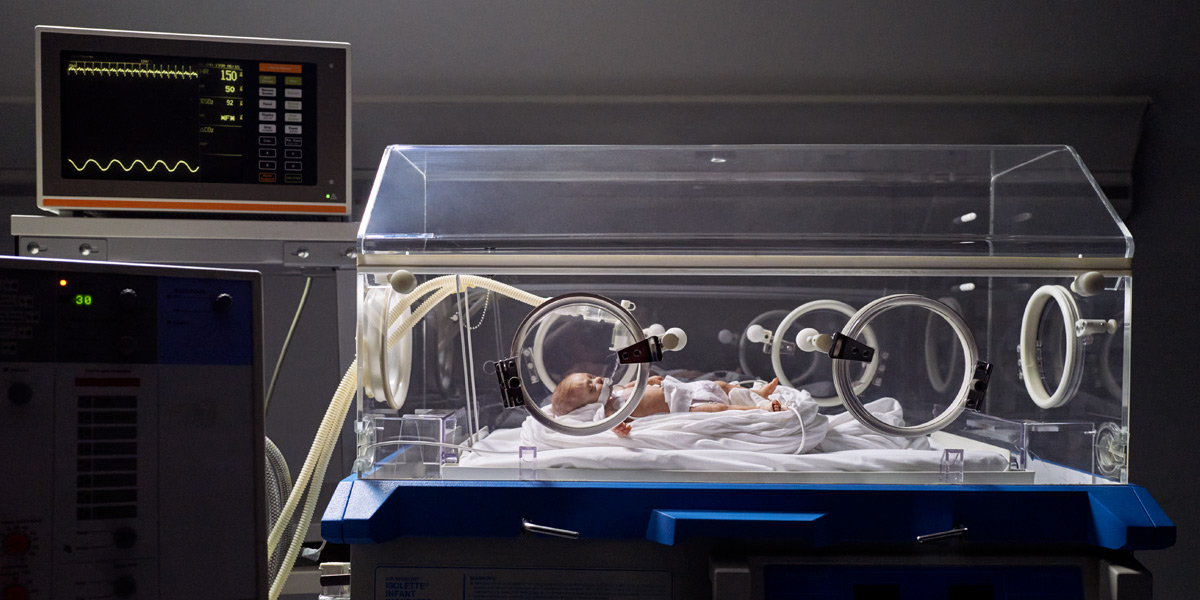
One ventilation technique that breathes with the patient is called Neurally Adjusted Ventilatory Assist, or NAVA, developed by Getinge, a global leader in intensive care technology for both infants and adults.
Before NAVA, ventilation technology had advanced to the point that a sensor in the breathing tube alerted when a baby was trying to breathe in, and the machine supplied a breath. But there was lag time, resulting in the machine sometimes not supplying air when the lungs called for it, or forcing air into frail lungs that were not ready for it—a problem amplified by premature babies' tendency to take short, rapid and uneven breaths.
"NAVA is a way to do a little better job," says Sherry Courtney, a director of clinical research in neonatology, who has worked with premature babies since the 1980's. "The diaphragm is a muscle. When it contracts, we're going to breathe. When it relaxes, we're going to exhale. So NAVA senses the breathing using a catheter that goes down into the stomach and rests close to the diaphragm."

Electrodes on the catheter sense contractions in the diaphragm, resulting in an almost instantaneous signal that the patient wants to breathe. Synchronously, the ventilator supplies air. And when the electrodes sense the end of diaphragmatic contractions, the ventilator allows exhalation.
"NAVA just provides a little support, depending on the breath. The patient can be breathing as the patient wishes. Deep breaths, shallow breaths, long breaths, short breaths, bigger volumes, smaller volumes. That's the way people breathe," says Courtney. "And NAVA may allow all of that to happen, along with making sure everything is synchronized to the pattern of the breathing. So it's a very useful way to ventilate because it increases the comfort for the patient." [7] [8]
Courtney says she's observed many babies who switch to a NAVA-enabled ventilator almost immediately become more comfortable and less irritable. Their oxygen needs decrease, as do pressure and volume requirements. Babies can be more restful and concentrate energy on the single most important thing they can do during their premature stage—grow.
We have been switching in our unit more and more to NAVA because the babies seem to love it.
What’s not so well known in the U.S. is that NAVA is also approved for adults, and the features that make the technique successful for neonates translate well to adult patients. Adults on ventilators generally start with a functioning diaphragm, but it will become weaker quickly if a machine breathes for them for too long. Getinge Medical Director Miray Kärnekull says that advanced ventilator technologies like NAVA are used regularly in adult patients in Europe to keep patients' diaphragm muscles active.

"With conventional ventilation modes there is no monitoring of the diaphragm activity. [1] [2] So you have no idea actually what's happening there," Kärnekull says. Driving too much air into the lungs, for instance, suppresses the respiratory drive and weakens the diaphragm. This can cause problems when it's time to wean a patient off the ventilator. [3] [4]
In addition to helping maintain the diaphragm's tone, the synchrony of a NAVA ventilator means patients don't fight against the ventilator. To prevent that, adults usually need to be heavily sedated. With NAVA, doctors can reduce sedatives, allowing for earlier weaning with fewer complications. [5] It’s really a groundbreaking technology. NAVA gives the clinician a way to personalize not only the ventilation, but also the weaning process for adult patients.[6]
And in a very recent multicenter randomized controlled trial, results showed that patients with acute respiratory failure placed on NAVA spent significantly less time on the ventilator and experienced less extubation failure compared to conventional lung-protective mechanical ventilation” [9].
NAVA technology is only one way ventilators are improving. Advances in the machines themselves, and the software that powers them, have allowed for more personalization. Critical care ventilators can now be fine-tuned to each patient's specific needs. David A. Kaufman, MD, Pulmonary & Critical Care Medicine at NYU School of Medicine in New York, says that advanced machines like Getinge's are able to convey much more information about the patient's condition.
"The 2020 advanced critical care ventilators give us flexibility, information, fabulous ways of measuring, on a moment-to-moment basis, very sophisticated levels of interaction between patient and ventilator," Kaufman says. "And what that really does, is help us tailor what we do to individuals in a very, very refined way. We like to be sure that we can meet each individual patient's needs as specifically as we can, and today's top-line ventilators really give us the tools to do that."

But some medical emergencies are too complicated and acute for even the most sophisticated ventilators. For those instances, another technological development has arisen to support the ventilation. This technique, called Extracorporeal Life Support (ECLS), simulates the function of lungs or a heart that has ceased working.
"Basically, we take blood out of one of the big veins in the body," Kaufman says. "We run it through a chamber where we are able to extract the carbon dioxide and put in a high concentration of oxygen. Then, that blood is injected back into another vein."
Invented in the 1960’s to facilitate cardiac surgeries with cardiopulmonary bypass, extracorporeal techniques and technologies have been refined to the point that they are used increasingly worldwide. In response, Getinge, a leading manufacturer of equipment used in extracorporeal support, has increased investment and production of components to meet demands.
ECLS is primarily a way to buy time and keep the blood oxygenated without damaging lungs in the most critical situations—like multi-organ failure—while doctors figure out how to save the patient. The technique has potential in the case of trauma, while a patient awaits organ donations, or in the treatment of acute respiratory distress, when a ventilator can cause damage.
"There are times when people have such sick lungs, they're so wet, they're so heavy, they're so stiff, that the force that a mechanical ventilator needs to apply to get any gas into the lungs is very high," Kaufman says.
ECLS allows us to make sure that we're not adding to the damage that's already occurring from the patient's underlying disease.
These high-tech medical procedures are a few of the developments changing the way that doctors practice intensive care medicine. Advanced monitoring provides far more real-time information than was ever before available. The flow of information and the increased use of artificial intelligence provide contextual information. The continued enablement of machines to communicate with each other will lessen the burden on staff and increase the ability of caregivers to focus more on the patient's needs in the moment.
These exciting advances have allowed physicians like Checketts to celebrate even more success stories. Checketts decided to become a doctor at early age, when her mother routinely pointed out a man walking down the street on his way to the hospital and said, "That’s the doctor who saved your life". That experience motivates her to be a positive force in the families of the babies she treats.
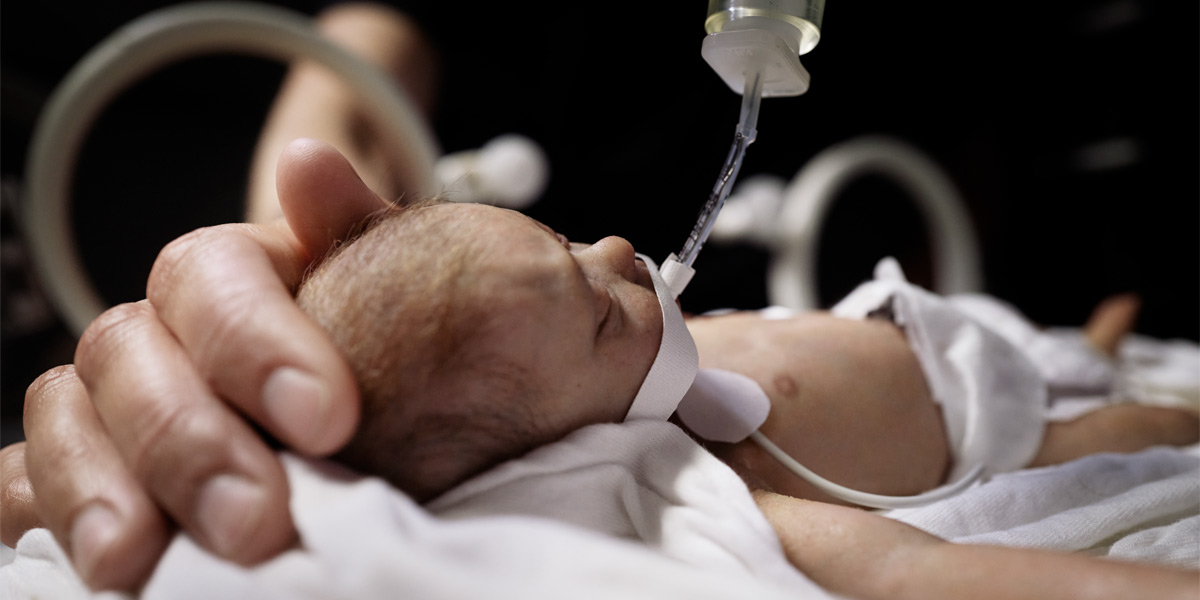
"When I talk to parents about the fact that I was premature, there's always a sense of surprise, I think a little bit even shock, you know. Oh, oh, and you're a doctor," Checketts says. "I think it's a nice way to say to them that prematurity shouldn't be a limit on what a child can do.”
"I mean, the advances we've made in even just the last 10, 15, 20 years mean the outcomes are much better than they used to be. Seeing me, who developed before that, as a newborn doctor, I give them a sense of hope and possibility, I think."