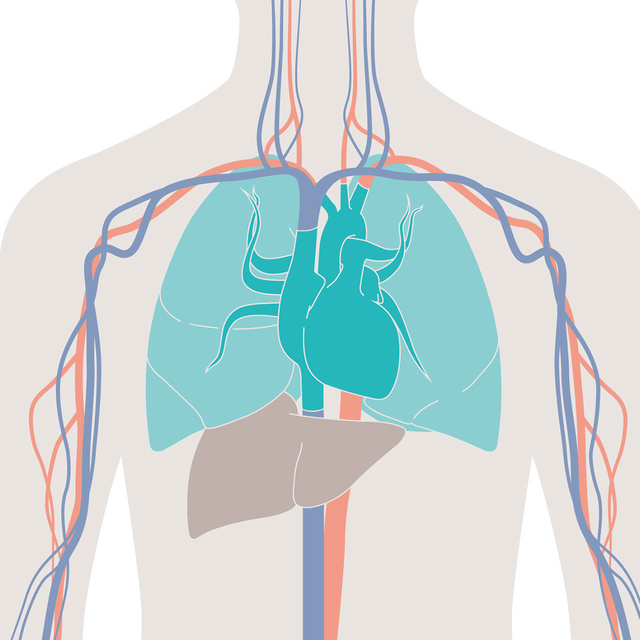
An easy, less invasive and cost-efficient tool
PiCCO helps determining the main hemodynamic parameters of critically ill patients
- Bedside quantification of pulmonary edema
- Quantification of cardiac preload
- Several arterial access points inc. for paediatric patients
- Precise, calibrated Cardiac Output – beat-to-beat
- Volumetric preload parameter instead of filling pressures
- Afterload, contractility, volume responsiveness

Understand complex conditions with PiCCO
The life of your critically ill patient depends on the right decision for the next therapeutic step. Therapeutic conflicts often arise at the critical care bedside, where you need dependable information you can trust. A set of reliable hemodynamic parameters can help determine the best individual treatment for your patients. [1] [2] [3] [4]
Main indications:
- Septic shock
- Cardiogenic shock
- Traumatic shock
- ARDS
- Severe burn injuries
- Pancreatitis
- High risk surgical procedures
The medical device is CE marked according to Directive 93/42/EEC.
Related products
Hemodynamic Monitoring at the highest level
Based on two physical principles
The PiCCO Technology combines arterial pulse contour analysis using the innovative PiCCO algorithm with precise calibration via transpulmonary thermodilution
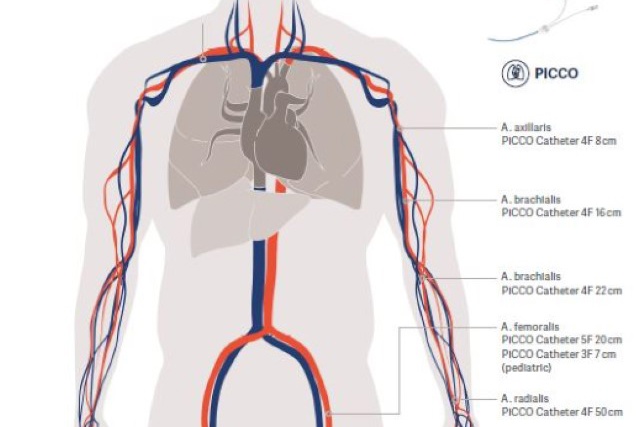
Arterial access
Via femoral, brachial and axillary artery
Children / paediatrics application
With special 3 french PiCCO catheter possible
Hemodynamic management of unstable patients

The PiCCO Module for PulsioFlex helps manage patient with unstable hemodynamic conditions
- The PiCCO Module upgrades the PulsioFlex monitor to the use of the PiCCO Technology
- PiCCO advances the precision and reliability of hemodynamic monitoring by calibration via transpulmonary thermodilution
- The PiCCO Module enables lung oedema diagnosis by measuring extravascular lung water
- The PiCCO parameters, including preload volume, volume responsiveness, afterload and contractility enable the doctor to apply patient centered treatments, including using inotropes and vasopressors
The medical device is CE marked according to Directive 93/42/EEC.
PiCCO Kit
The best and safest way of using the technology is to use the complete kit
These consist of:
- PiCCO Catheter with Seldinger insertion instruments, guide wire, canula, dilatator and
- PiCCO Monitoring Kit with injectate sensor housing and pressure transducer
*Picture shows recommended application sites

Full functionality for IntelliVue
The PiCCO Technology is also available with full functionality as an integrated module for IntelliVue and CMS Patient Monitors from Philips Medical Systems. For more information about the module, please go to our partnership page or directly to Philips.
Technical specifications are subject to change without further notice
PiCCO practical help
Find out more how to optimize PiCCO thermodilution measurements in daily use
Containing comprehensive practical support, the PiCCO Trouble Shooting Guide assists clinicians and technicians when in need for handling information.

Two components of the PiCCO technology
The PiCCO technology is based on two physical principles, namely transpulmonary thermodilution and pulse contour analysis. Both principles allow the calculation of haemodynamic parameters and have been clinically tested and established for more than 20 years.
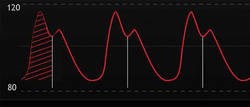
Arterial pulse contour analysis
The pulse contour analysis provides continuous information while transpulmonary thermodilution provides static measurements. Transpulmonary thermodilution is used to calibrate the continuous pulse contour parameters.
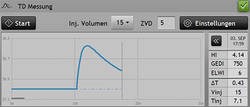
Transpulmonary thermodilution
For the transpulmonary thermodilution measurement, a defined bolus (for example 15mls cold 0.9% normal saline) is injected via a central venous catheter. The cold bolus passes through the right heart, the lungs and the left heart and is detected by the PiCCO catheter, commonly placed in the femoral artery. This procedure should be repeated around three times in under 10 minutes to ensure an accurate average is used to calibrate the device and to calculate the thermodilution parameters. These thermodilution parameters (i.e. they are updated only when the thermodilution procedure is performed) should be checked whenever there is a significant change in the patient’s condition or therapy. It is recommended to calibrate the system at least 2 to 3 times per day depending on the patients condition.
Marketing Sales - Brochures
-
Clinical evidence for PiCCO Technology, studies, outcomes and review articles about PiCCO Technology. Cost effectiveness, validation and significance of PiCCO Catheter parameters. Recommended clinical application areas, clinical and medical questions, technique and technology questions
Visit our Academy – training and education designed to enhance your proficiency
For more information about our onsite events or remote trainings, you can also contact your local sales & service representative.